In April, 2019, new research from the Brigham and Women’s Hospital and Harvard Medical School in Boston, MA,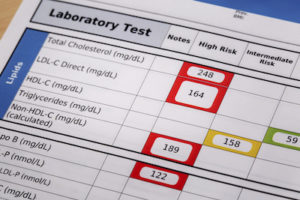 
“Women already have a higher risk of stroke than men, in part because they live longer, so clearly defining ways to reduce their risk is important.” ~ study author Pamela Rist, from Brigham and Women’s Hospital.
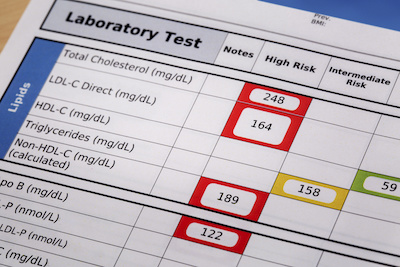
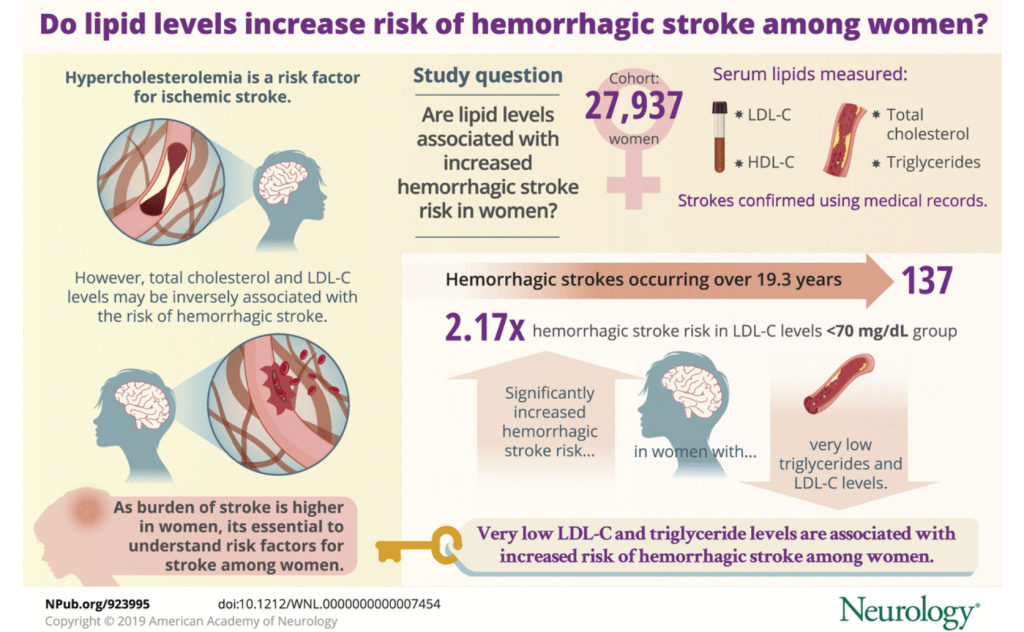
Let’s start with the results. The researchers performed a prospective cohort study among 27,937 women enrolled in the Women’s Health Study with measured total cholesterol, low-density lipoprotein cholesterol (LDL-C), and high-density lipoprotein cholesterol (HDL-C), as well as triglycerides. Strokes were confirmed by medical record review. Cox proportional hazards models were used to analyze associations between lipid categories and hemorrhagic stroke risk.
During a mean of 19.3 years of follow-up, 137 hemorrhagic strokes occurred. Compared to those with LDL-C levels 100–129.9 mg/dL, after multivariable adjustment, those with LDL-C levels <70 mg/dL had 2.17 times the risk (95% confidence interval [CI] 1.05, 4.48) of experiencing a hemorrhagic stroke. No significant increase in risk was seen for those with LDL-C levels 130–159.9 mg/dL (relative risk [RR] 1.14; 95% CI 0.72, 1.80) or 70–99.9 mg/dL (RR 1.25; 95% CI 0.76, 2.04).
There was a suggestion, although not significant, of increased risk for those with LDL-C levels ≥160 mg/dL (RR 1.53; 95% CI 0.92, 2.52). Women in the lowest quartile of triglycerides had a significantly increased risk of hemorrhagic stroke compared to women in the top quartile after multivariable adjustment (RR 2.00; 95% CI 1.18, 3.39). The researchers observed no significant associations between total cholesterol or HDL-C levels and hemorrhagic stroke risk.
According to Dr. Klodas, what should physicians do with this new information?
This study may leave patients perplexed about their ideal LDL cholesterol numbers. Hemorrhagic strokes are 
“Not surprisingly, these findings generated a lot of press coverage, raising concerns among many patients who are purposefully trying to lower their LDL,” said Dr. Klodas. “Noteworthy is the fact that published cholesterol treatment guidelines actually advise getting LDL to below 70 mg/dL if heart disease is present.”
The following is a review of the study by Dr. Klodas:
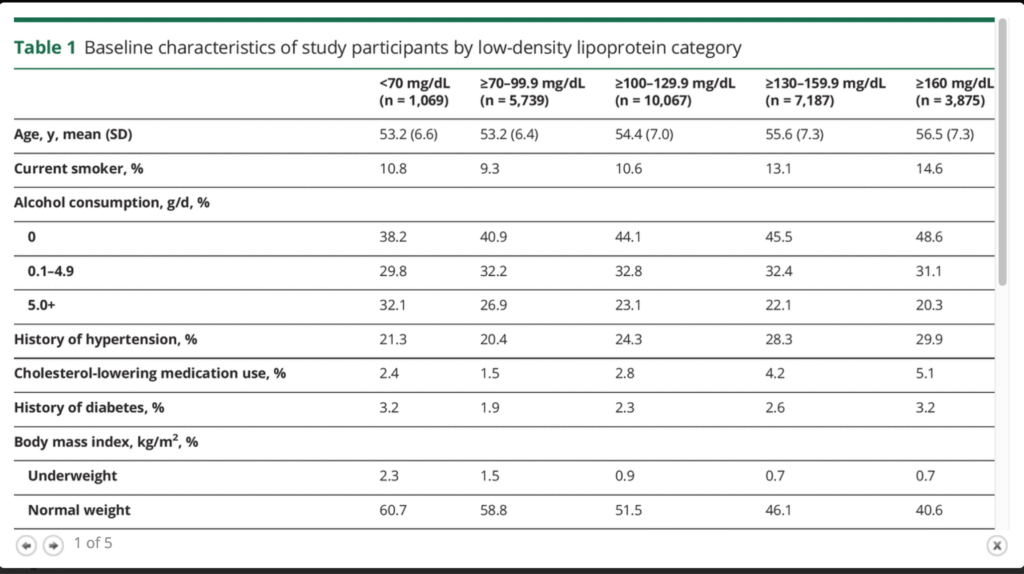
1. Over the 19 years of the study, only 0.8% of women with very low LDL experienced a hemorrhagic stroke, compared to 0.4% of women with higher LDL readings. So the rate of events might have doubled with low LDL values, but practically speaking the chance of experiencing a bleeding stroke is still remote, regardless of cholesterol level. And just in case you’re wondering, for triglycerides, 0.6% of women with levels below 74 mg/dL experienced a stroke, compared to 0.4% of those with higher levels.
2. The researchers only looked at the very first cholesterol profile obtained at the beginning of the study. And we don’t know what happened to those profiles over time. If some of the women with higher LDL levels ended up with lower readings during the 19 years of follow-up (because they were placed on statins, for example), the whole premise of the analysis could have been made moot.
3. Women with migraine headache with aura, and women with a past history of high blood pressure with pregnancy (preeclampsia) have also been shown to have increased risk for hemorrhagic stroke and these risk factors were not accounted for in comparing the groups.
4. Most notably, it’s the cumulative risk of all events that matters, so don’t forget the bigger picture. Especially since multiple other large studies have shown improved overall outcomes with lower LDL readings.
So what is Dr. Klodas telling her patients?
“The same thing I’ve been telling them all along. That people who live long well do so because they live well – and achieving perfect numbers without achieving a better lifestyle is an incomplete solution. And that one study, regardless of how many people were enrolled, doesn’t change the fundamentals. And that the risk of a bleeding stroke is very low regardless of cholesterol levels. And that, based upon mountains of evidence, LDL under 70 mg/dL is still a reasonable goal for those individuals who have established heart disease.”
Source: Pamela M. Rist, Julie E. Buring, Paul M Ridker, Carlos S. Kase, Tobias Kurth, Kathryn M. Rexrode, Lipid levels and the risk of hemorrhagic stroke among women. Neurology May 2019, 92 (19) e2286-e2294; doi: 10.1212/WNL.0000000000007454