People infected with COVID-19 experience a wide range of symptoms and severity, including high fevers and respiratory problems. However, new research shows that when the virus attacks the gastrointestinal tract, it may increase the severity of the viral infection. The research review, published in mBio, suggests that gut dysfunction and associated leaky gut may enable the virus to access the surface of the digestive tract and internal organs, which are vulnerable to infection because they have widespread ACE2, a protein target of SARS-CoV-2–on the surface.
“There seems to be a clear connection between the altered gut microbiome and severe COVID-19,” said microbiologist Heenam Stanley Kim, Ph.D, from Korea University’s Laboratory for Human-Microbial Interactions, in Seoul.
Studies have demonstrated that people with underlying medical conditions including high blood pressure, diabetes and obesity face a higher risk of severe COVID-19. Risk also increases with age, with older adults most vulnerable to the most serious complications and likelihood of hospitalization. But both of the factors of advanced age and chronic conditions have a well-known association with an altered gut microbiota. This imbalance can affect gut barrier integrity, Kim noted, which can allow pathogens and pathobionts easier access to cells in the intestinal lining.
So far, the link between gut health and COVID-19 prognosis hasn’t been empirically demonstrated, Kim noted. Some researchers have argued, he said, that unhealthy gut microbiomes may be an underlying reason for why some people have such severe infections.
What studies have been done hint at a complicated relationship. Study highlights include:
- A study on symptomatic COVID-19 patients in Singapore, for example, found that about half had a detectable level of the coronavirus in fecal tests, but only about half of those experienced GI symptoms. That study suggests that even if SARS-CoV-2 reaches the GI tract, it may not cause problems. Kim also noted that a person’s gut health at the time of infection may be critical for symptom development.
- Many recent studies have found reduced bacterial diversity in gut samples collected from COVID-19 patients, compared to samples from healthy people.
- The disease has also been linked to a depletion of beneficial bacterial species – and the enrichment of pathogenic ones. A similar imbalance has been associated with influenza A infection, though the 2 viruses differ in how they change the overall microbial composition.
- The depleted bacterial species associated with COVID-19 infection include some families that are responsible for producing butyrate, a short-chain fatty acid, which plays a pivotal role in gut health by reinforcing gut-barrier function.
Is the Western Diet a Factor in Disease Severity?
Kim said he started analyzing the studies after realizing that wealthy countries with a good medical infrastructure–including the United States and nations in Western Europe–were among the hardest hit by the virus. The “western diet” that’s common in these countries is low in fiber, and “a fiber-deficient diet is one of the main causes of altered gut microbiomes,” he said, “and such gut microbiome dysbiosis leads to chronic diseases.”
The pathogenesis of COVID-19 is still not fully understood. If future studies do show that gut health affects COVID-19 prognosis, Kim argued, then clinicians and researchers should exploit that connection for better strategies aimed at preventing and managing the disease. Eating more fiber, he said, may lower a person’s risk of serious disease. And fecal microbiota transplantation might be a treatment worth considering for patients with the worst cases of COVID-19.
The problem with gut health goes beyond COVID-19, though, he said. Once the pandemic passes, the world will still have to reckon with chronic diseases and other problems associated with poor gut health.
“The whole world is suffering from this COVID-19 pandemic,” Kim said, “but what people do not realize is that the pandemic of damaged gut microbiomes is far more serious now.”
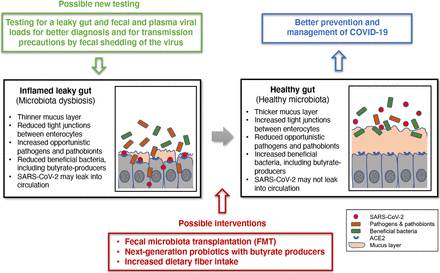
Conclusion/ The researchers conclude: “A strong pattern has emerged from patients with severe COVID-19, as many of them are either elderly or have certain underlying medical conditions which may be associated with an altered gut microbiota. Such dysbiosis of the gut microbiota may be associated with disrupted gut barrier integrity, which may allow SARS-CoV-2 to gain access to the otherwise well-protected enterocytes and to circulate and infect internal organs expressing ACE2. If this is what is happening in the serious cases of this illness that present extrapulmonary multiorgan dysfunction, testing for a leaky gut and fecal and plasma viral loads will be of high value for a more accurate prognosis, particularly for those likely to have altered gut microbiotas. Furthermore, fecal viral load data can also be useful for informing transmission precautions, because some patients may have prolonged fecal shedding of the virus even after viral clearance in the respiratory tract.”
Click Here for Full Text Study