As many as 25% of Americans suffer from dry eyes or a related abnormality of the ocular surface. As this pilot study shows, a combination treatment of warm heat compresses and an Omega-3 fatty acid supplement can be an effective treatment option for dry eye disease (DED). Published in Alternative Therapies, by Will Smith, OD; David McMahon, MBA, MS; Maria Nymark, PhD.
This 4-week study included 35 participants (33 completed the trial), age 18-75 with an ocular surface disease, Meibomian gland disease (MGD). In the eye, Meibomian glands secrete a lipid and protein mixture, which creates a clear optical surface for the cornea. It also prevents bacterial colonization and tear overflow. The liquid secretion also improves stability and reduces the evaporation of the tear film. When the MGD dysfunctions it destabilizes the tear film, resulting in increased evaporation and osmolarity.
The study authors note,
MGD exerts a significant effect on gene expression in the human Meibomian gland. These changes, which have not been accounted for by gender-associated differences between control and MGD patient populations, are accompanied by upregulation and downregulation of many processes (ie, keratinization, the cell-division cycle, DNA repair, and the formation of cytoplasmic vesicles and cornified envelope components).5,6 MGD is often considered to be a key instigator of DED and should be targeted to reduce both symptoms and degenerative processes related to dry eye.
Warm compresses are a common treatment for MGD, as the heat “causes the meibum to become less viscous and minimizes meibomian gland obstruction and inspissation.” When combined with a therapeutic dose of Omega-3 fatty acids, the benefits are notable. Previous studies show regular intake of Omega-3 fatty acids can:
- Decrease in artificial tear use,
- Reduce conjunctival hyperemia,
- Improve tear secretion, and tear film stability.
DRY EYES TREATMENT PROTOCOL
In this 30-day study, patients were asked to use a warm eye compress, heated for 30 seconds in the microwave and apply it to closed eyes for 5 minutes daily. They also took an Omega-3 softgel that contained 810 mg of omega-3 polyunsaturated fatty acids in the rTG form with 390 mg of eicosapentaenoic acid (EPA) and 193 mg of acid docosahexaenoic acid (DHA) (download the full study for more information on the Omega-3 supplement).
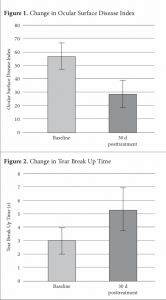
More than half of the enrolled patients (54%) were considered to have severe DED based on the OSDI scoring, with a mean starting score of 57 ± 19.3 (Figure 1). Participants showed significant improvements between baseline and post intervention, demonstrated by a decrease in OSDI scores of 28 points (49%) to an average of 29 ± 21.1, with P = .0015. Furthermore, 45% of patients reported becoming asymptomatic of dry eye symptoms.
By prescribing what the researchers call, “a very conservative and efficient protocol of fewer than 7 minutes per day,” they were able to reduce symptoms of DED significantly and to offer a low-risk therapy for patients and clinicians. The researchers concluded, “because DED is a chronic disease, the ease of use of the proprietary Dry Eye Protocol may enable better long-term dry eye management by improving patients’ compliance. Patients’ education in DED and understanding of the best strategy for the individual is imperative in achieving long-term success in overcoming this epidemic.”