Veterans who have acupuncture before surgery report less pain and need far fewer opioids to manage their discomfort, according to a randomized, controlled study being presented at the ANESTHESIOLOGY® 2020 annual meeting. Veterans who received acupuncture also reported they were more satisfied with their pain control than those who did not.
“Six percent of patients given opioids after surgery become dependent on them, and Veterans are twice as likely to die from accidental overdoses than civilians,” said Brinda Krish, D.O., lead author of the study and an anesthesiology resident at Detroit Medical Center, “Clearly it is crucial to have multiple options for treating pain, and acupuncture is an excellent alternative. It is safe, cost effective and it works.”
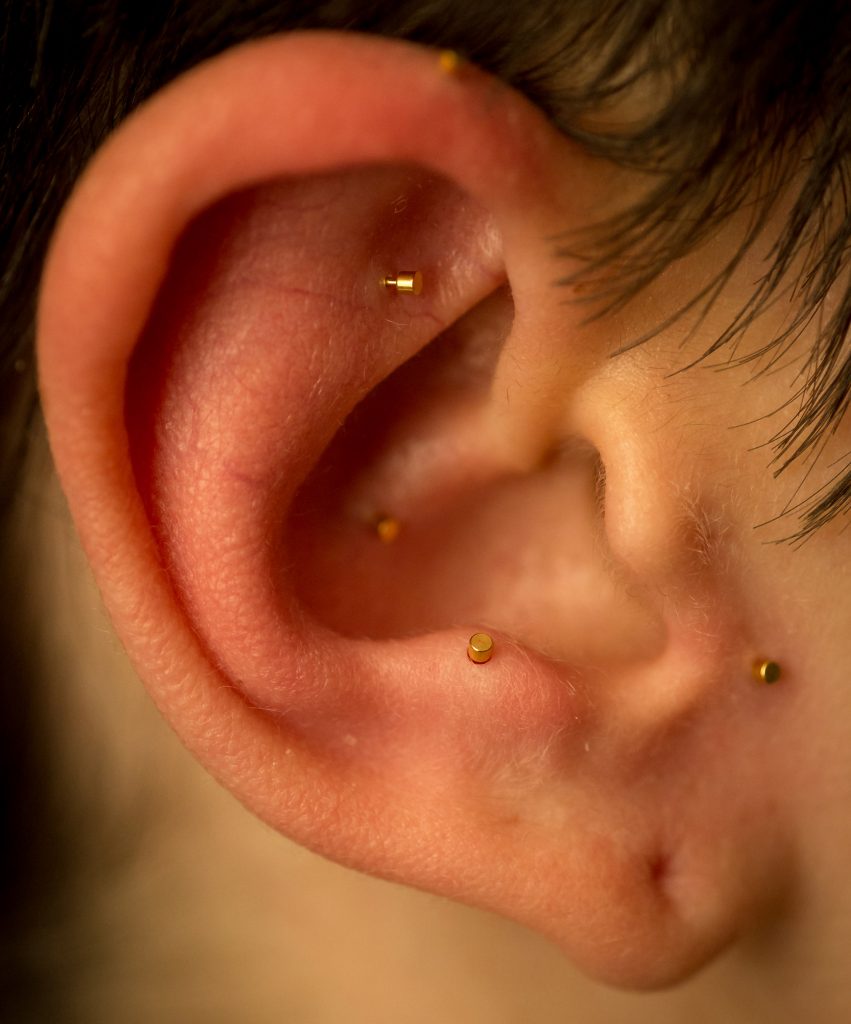
In the study, both traditional and battlefield acupuncture were used. Traditional acupuncture involves the insertion of very thin needles at specific trigger points around the body to relieve pain. Battlefield acupuncture, developed by a U.S. Air Force doctor to reduce pain without the use of opioids on the front lines, uses tiny needles that are inserted at various trigger points in the ear.
Researchers included two groups of patients treated at John D. Dingell VA Medical Center in Detroit.
- One group received hip replacement surgery and were randomly assigned to either traditional acupuncture or a control group before surgery;
- and the other included patients undergoing a variety of surgeries (including gallbladder removal, hernia repair, hysterectomy or prostate surgery) who were randomly assigned to receive battlefield acupuncture or to a control group before surgery.
In the first group, 21 patients had traditional acupuncture and 21 were in the control group.
- Those who had traditional acupuncture consumed an average of 20.4 of morphine milligram equivalent (MME) in the first 24 hours after surgery.
- Patients in the control group consumed 56 MME, nearly three times as much.
- Traditional acupuncture patients reported significantly higher satisfaction scores regarding their postoperative pain management 24 hours after surgery (median 8 vs. 5).
- Patient satisfaction was estimated using a scale (0-10) – with 10 being completely satisfied. Acupuncture patients reported less pain and 14% reported less anxiety.
In the second group, 28 patients received battlefield acupuncture and 36 patients were in the control group.
- Those who had battlefield acupuncture consumed half as many opioids in the first 24 hours after surgery compared to the control group: 17.4 MME vs. 35 MME.
- Those who received battlefield acupuncture had significantly lower pain scores and higher patient satisfaction scores (a median of 8 vs. 6) compared to the control group.
- Only 3% reported nausea and vomiting after surgery, compared to 38% of the control group.
- Researchers believe nausea and vomiting may have been reduced in the treatment group because some of the acupuncture points in the ear are located near trigger points for the stomach, gall bladder and small intestines.
“Some patients were open to trying acupuncture right away, and others became more interested when they learned more about the risks of opioid use,” said Dr. Krish. “It’s easy, patients love it, it’s not just another medicine and it’s very safe. Because battlefield acupuncture was developed by an armed services doctor, Veterans also were more willing to participate.”
The acupuncture was provided by the study’s principal investigator, physician anesthesiologist Padmavathi Patel, M.D., D.ABA, who plans to use battlefield acupuncture as an additional therapy for pain management for all patients receiving general anesthesia, Dr. Krish said.




