Glucosamine is a popular non-vitamin, non-mineral supplement widely used for osteoarthritis and joint pain. While the effectiveness of glucosamine in patients with osteoarthritis and joint pain is well known, emerging evidence from epidemiological studies suggests that glucosamine could have a role in preventing cardiovascular disease (CVD) and reducing mortality.
A previous animal study reported that glucosamine extended life span by mimicking a low carbohydrate diet, and 
In this prospective cohort study, researchers examined the association between habitual glucosamine supplement use and risk of CVD events (CVD death, coronary heart disease (CHD), and stroke) in nearly half a million adults in the UK Biobank. We also analyzed potential effect modification by other known risk factors for CVD. Data from 502,616 participants were available for the study. Participants with CVD at baseline (n=32 187) were excluded and those with incomplete data on the use of glucosamine (n=4390). The final analysis included 466,039 participants.
We used the baseline touch screen questionnaire to assess several potential confounders: age, sex, race, household income, smoking status, and alcohol intake (we calculated ethanol intake by multiplying the quantity of each type of drink—red wine, white wine, beer or cider, fortified wine, or spirits—by its standard drink size and reference alcohol content); self reported diabetes and high cholesterol level; drugs to treat high cholesterol, high blood pressure, and diabetes; aspirin and other non-steroidal anti-inflammatory drug use; and dietary intakes (red meat, vegetables, fruit, fish, and cereals). One point was assigned for each favorable diet factor, and the total diet score ranged from 0 to 6. A healthy diet was defined as a diet score of 3 or more.
The ion selective electrode method (AU5400 analyzer, Beckman Coulter) was used to measure sodium levels in stored urine samples. The analytic range for sodium was 2-200 mmol/L. Participants were categorized into two groups based on total moderate physical activity minutes each week (one vigorous physical activity minute equals two moderate physical activity minutes): <150 or ≥150 min/week. Hypertension was defined as a self reported history of hypertension, systolic blood pressure of 140 mm Hg or higher, diastolic blood pressure of 90 mm Hg or higher, or taking antihypertensive drugs. Arthritis was defined by ICD-10 (international classification of diseases, 10th revision) codes M15-M19.
In this large prospective study, habitual glucosamine use was associated with a 15% lower risk of total CVD events and a 9%-22% lower risk of individual cardiovascular events (CVD death, CHD, and stroke). Such associations were independent of traditional risk factors, including sex, age, income, body mass index, physical activity, healthy diet, alcohol intake, smoking status, diabetes, hypertension, high cholesterol, arthritis, drug use, and other supplement use. In addition, we found that the associations between glucosamine use and CVD outcomes were statistically significantly modified by smoking status.
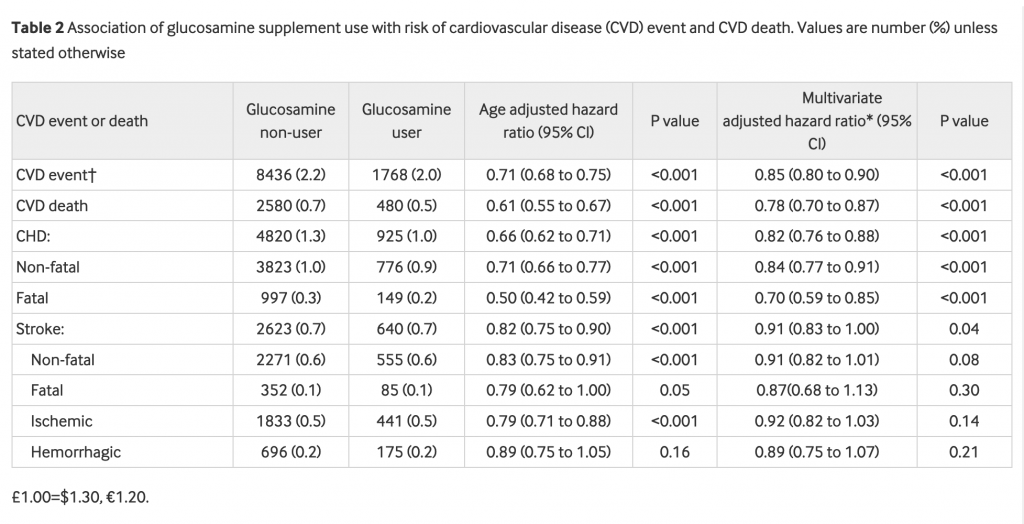
Conclusion/ Habitual use of glucosamine supplement to relieve osteoarthritis pain might also be related to lower risks of CVD events. Further clinical trials are needed to test this hypothesis.
Click Here for Full Text Study
Source: Ma Hao, Li Xiang, Sun Dianjianyi, Zhou Tao, Ley Sylvia H, Gustat Jeanette et al. Association of habitual glucosamine use with risk of cardiovascular disease: prospective study in UK Biobank BMJ 2019; 365 :l1628