A recent study in Clinical Nutrition study, published July 2017, is providing further evidence of the value of personalized nutrition and nutrigenomics. Researchers studied whether dietary linoleic acid (LA) or α-linolenic acid (ALA) can modulate the expression of genes that influence lipid and anthropometric phenotypes. This meta-analysis of 3069 French adults showed that for subjects with high LA consumption, who carry the rs174547 minor allele, there was a significant association with higher HDL-cholesterol levels, higher body mass index and higher waist circumference.
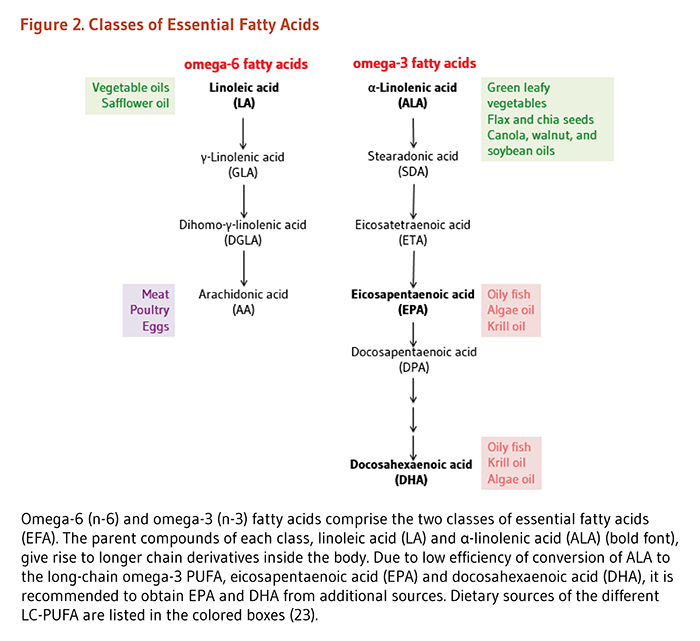
Dietary linoleic acid (LA) is one of the most abundantly consumed forms of Omega-6 fatty acids as it accounts for 90% of the polyunsaturated fatty acids in the diet. Common sources include vegetable oils used in processed food production (see Figure 2). Experts have long raised the question of how much LA should be consumed daily and warned about the ill effects of high consumption. This latest study further confirms that for some individuals with particular genomic profiles, high LA intake could have a detrimental affect on cardiovascular health and weight management goals.
Background on Dietary Linoleic Acid Study
Blood levels of polyunsaturated fatty acids (PUFAs) are under control of endogenous synthesis via Δ5- and Δ6-desaturases, encoded by the FADS1 and FADS2 genes, respectively and of diet. Genome-wide associations studies (GWAS) reported associations between polymorphisms in FADS1–FADS2 and variations in plasma concentrations of PUFAs, HDL- and LDL-cholesterol and triglycerides. However, it is not established whether dietary PUFAs intake modulates these associations. We assessed whether dietary linoleic acid (LA) or α-linolenic acid (ALA) modulate the association between the FADS1 rs174547 polymorphism (a GWAS hit) and lipid and anthropometric phenotypes.
Methods
Dietary intakes of LA and ALA, FADS1 rs174547 genotypes, lipid and anthropometric variables were determined in three French population-based samples (n = 3069). These samples were stratified according to the median dietary LA (<9.5 and ≥9.5 g/d) and ALA (<0.80 and ≥0.80 g/d) intakes. The meta-analysis was performed using a random-effect.
Results
The meta-analysis confirmed the association between rs174547 and plasma lipid levels and revealed an association with waist circumference and body mass index. These associations were not modified by dietary ALA intake (all p-interaction > 0.05). In contrast, the associations with HDL-cholesterol levels, waist circumference and BMI were modulated by the dietary intake of LA (p interaction < 0.05).
In high LA consumers only, the rs174547 minor allele was significantly associated with lower HDL-cholesterol levels (β = −0.05 mmol/L, p = 0.0002). Furthermore, each copy of the rs174547 minor allele was associated with a 1.58 cm lower waist circumference (p = 0.0005) and a 0.46 kg m−2 lower BMI (p = 0.01) in the low LA intake group, but not in the high LA intake group.
Conclusions
The present study suggests that dietary LA intake may modulate the association between the FADS gene variants and HDL-cholesterol concentration, waist circumference and BMI. These gene–nutrient interactions, if confirmed, suggest that subjects carrying the rs174547 minor allele might benefit from low dietary LA intakes.
Link here for access to Clinical Nutrition and the study registration page.





