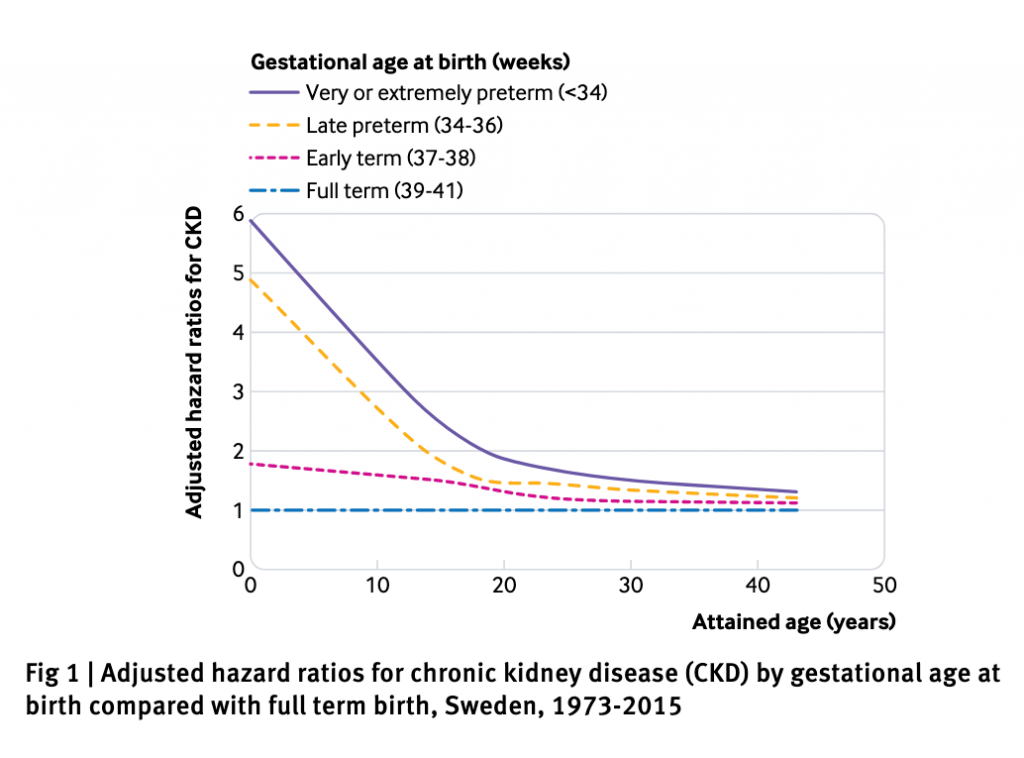
Preterm and early term birth are strong risk factors for the development of chronic kidney disease (CKD) from childhood into mid-adulthood, suggests a study from Sweden published by The BMJ. Given the high levels of preterm birth (currently 10% in the US and 5-8% in Europe), and better survival into adulthood, these findings have important public health implications, say the researchers.
Preterm birth (before 37 weeks of pregnancy) interrupts kidney development and
maturity during late stage pregnancy, resulting in fewer nephrons forming (filters that remove waste and toxins from the body). Lower nephron number has been associated with the development of high blood pressure and progressive kidney disease later in life, but the long-term risks for adults who were born prematurely remain(ed) unclear.
A team led by Professor Casey Crump at the Icahn School of Medicine at Mount Sinai in New York, set out to investigate the relation between preterm birth and risk of CKD from childhood into mid-adulthood.
Using nationwide birth records, they analyzed data for over 4 million single live births in Sweden during 1973-2014. Cases of CKD were then identified from nationwide hospital and clinic records through 2015 (maximum age 43 years). Overall, 4,305 (0.1%) of participants had a diagnosis of CKD, yielding an overall incidence rate of 4.95 per 100,000 person years across all ages (0-43 years).
After taking account of other factors that might be important, they found that preterm birth (less than 37 weeks) was associated with a nearly twofold increased risk of CKD into mid-adulthood (9.24 per 100,000 person years). Extremely preterm birth (less than 28 weeks) was associated with a threefold increased risk of CKD into mid-adulthood (13.33 per 100,000 person years). A slightly increased risk (5.9 per 100,000 person years) was seen even among those born at early term (37-38 weeks).
The association between preterm birth and CKD was strongest up to age 9 years, then weakened but remained increased at ages 10-19 years and 20-43 years.
These associations affected both males and females and did not seem to be related to shared genetic or environmental factors in families. An increased risk was observed even among those born at early term (37-38 weeks) (1.30, 1.20 to 1.40; P<0.001). The association between preterm birth and CKD was strongest at ages 0-9 years (5.09, 4.11 to 6.31; P<0.001), then weakened but remained increased at ages 10-19 years (1.97, 1.57 to 2.49; P<0.001) and 20-43 years (1.34, 1.15 to 1.57; P<0.001). The study did not look as CKD risk beyond age 43.
The researchers emphasize that people born prematurely need long term follow-up for monitoring and preventive actions to preserve renal function across the life course. Clinical recommendations to preserve renal function in people born prematurely:
- Include birth history in medical history taking in patients of all ages, including adults, to help trigger preventive actions in those born prematurely
- Counsel patients on avoidance of potentially nephrotoxic exposures (eg, non-steroidal anti-inflammatory drugs) and other exacerbating factors (dehydration, recurrent urinary tract infections)
- Maintain well controlled blood pressure
- Reduce other known risk factors for chronic kidney disease, including obesity, diabetes, dyslipidemia, anemia, and smoking
- Periodically monitor renal function with serum creatinine, cystatin C, or urine albumin, based on individualized risk assessment
- For potential living kidney donors, advise caution because of higher susceptibility to renal dysfunction in the remaining kidney
This is an observational study, and as such, can’t establish cause, and the researchers acknowledge some limitations, such as a lack of detailed clinical data to validate CKD diagnoses and potential misclassification of CKD, especially beyond childhood. And they call for additional studies to assess these risks in later adulthood, and to further explain the underlying causes and clinical course of CKD in those born prematurely.
Click Here for Full Text Study