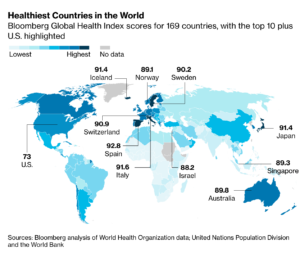
 Spain just surpassed Italy at the healthiest country in the world, according to the recent Bloomberg Healthiest Country Index. Must be the Mediterranean Diet (MeDi), say researchers. A new neuroimaging study shows that compliance to the MeDi is a critical factor in reducing the risk of cerebral Aβ-amyloid accumulation, a key factor in the development of Alzheimer’s Disease (AD).
Spain just surpassed Italy at the healthiest country in the world, according to the recent Bloomberg Healthiest Country Index. Must be the Mediterranean Diet (MeDi), say researchers. A new neuroimaging study shows that compliance to the MeDi is a critical factor in reducing the risk of cerebral Aβ-amyloid accumulation, a key factor in the development of Alzheimer’s Disease (AD).
Previous studies showed lower cognitive decline and reduced risk of Alzheimer’s were associated with the MeDi. However, relatively few studies have examined the relationship of MeDi adherence to AD-related neuroimaging outcome measures.
“Higher adherence to MeDi has been associated with greater cortical thickness, whilst similarly, lower MeDi adherence has been shown to be predictive of increased total brain atrophy.”
The aim of this current study was to assess the relationship between MeDi adherence, MeDi components, and Pittsburgh Compound B positron emission tomography (PiB-PET) determined cerebral Aβ burden longitudinally, in cogni- tively normal healthy control participants of the Australian Imaging, Biomarkers and Lifestyle (AIBL) Study of Ageing, who were categorised as “Aβ accumulators,” and thus considered to be on the AD pathway.
This study included data from 77 participants taken from the AIBL Study of Ageing who were classified as healthy controls (cognitively ‘normal’) and completed the Cancer Council of Victoria Food Frequency Questionnaire (CCVFFQ) at baseline, and who were categorized as “Aβ accumulators” as determined by PiB-PET imaging.
The CCVFFQ assigned a value of 1 for; (1) each beneficial component (fruits, vegetables, legumes, cereals and  fish) if caloric- adjusted consumption was at or above the cohort sex- specific median; (2) each detrimental component (meat and dairy) if caloric-adjusted consumption was below the sex-specific median; and (3) a ratio of monounsaturated to saturated fats at or above the median. Individuals were assigned a value of 1 for mild-to-moderate alcohol consumption (>5 to <25 g per day for females and >10 to <50 g per day for males). A MeDi score was subsequently generated for each participant by summing the scores for each category; MeDi score ranged from 0–9, with higher score indicating greater adherence.
fish) if caloric- adjusted consumption was at or above the cohort sex- specific median; (2) each detrimental component (meat and dairy) if caloric-adjusted consumption was below the sex-specific median; and (3) a ratio of monounsaturated to saturated fats at or above the median. Individuals were assigned a value of 1 for mild-to-moderate alcohol consumption (>5 to <25 g per day for females and >10 to <50 g per day for males). A MeDi score was subsequently generated for each participant by summing the scores for each category; MeDi score ranged from 0–9, with higher score indicating greater adherence.
The cohort comprised 77 cognitively normal healthy control “Aβ accumulator” participants (51% male) with an average age of 71.1 ± 7.1 years. Forty-two per cent were carriers of at least one APOE ε4 allele (the most common genetic risk factor for AD) and more than half had 13 or more years of education. The median MeDi score of the cohort was 4 (interquartile range 2) and 65% of participants had an standardized uptake value ratio (SUVR) less than 1.4 at baseline.
- The authors reported reduced cerebral Aβ load among individuals with high MeDi adherence.
- In the cohort, each one point MeDi score increase was associated with a 0.01 SUVR unit decrease in the accumulation of Aβ over three years; i.e., an individual who increased their MeDi adherence from 0 to 9 could potentially demonstrate a 0.09 SUVR unit decrease in the accumulation of Aβ over three years compared to a 0.01- unit decrease if they increased their MeDi adherence from 0 to 1.
- Higher fruit intake was associated with less accumulation of Aβ. Whilst the potential mechanism is unclear, researchers speculate that it may related to polyphenolic content.
- While the researchers cannot make a direct correlation between Aβ production and clearance, the researchers believe that vitamin A intake may play a role. The MeDi is an abundant source of vitamin A (both preformed vitamin A: retinol and its esterified form, retinyl ester, found in foods from animal sources, including dairy products, fish, and meat; and pro-vitamin A carotenoids, found in plant pigments), which has been shown to demonstrate anti-oligomerization effects on Aβ in vitro.
- The high concentration of vitamin C in fruits consumed as part of the MeDi (e.g. oranges, grapefruit and strawberries) may also contribute to slowing accumulation of cerebral AD pathology. Vitamin C supplementation has been shown to reduce amyloid plaque burden in the brain of a transgenic mouse model of AD, which had been genetically engineered to be unable to synthesize its own vitamin C (important as the ability of rodents to synthesize vitamin C with no reliance on dietary supply has hampered previous investigations). Moreover, vitamin C has been shown to inhibit amyloid fibril formation in vitro.
Conclusion/ This is the first study to assess the relationship between MeDi adherence and change in cerebral Aβ burden over time in older adults. In summary, the results of this study highlight the potentially beneficial impact of MeDi adherence on slowing rates of cerebral Aβ accumulation in cognitively unimpaired older adults.
Click Here for Full Text Study
Source: Rainey-Smith SR, Gu Y, Gardener SL, Doecke JD, Villemagne VL, Brown BM, Taddei K, Laws SM, Sohrabi HR, Weinborn M, Ames D, Fowler C, Macaulay SL, Maruff P, Masters CL, Salvado O, Rowe CC, Scarmeas N, Martins RN. Mediterranean diet adherence and rate of cerebral Aβ-amyloid accumulation: Data from the Australian Imaging, Biomarkers and Lifestyle Study of Ageing. Transl Psychiatry. 2018 Oct 30;8(1):238. doi: 10.1038/s41398-018-0293-5. PubMed PMID: 30375373; PubMed Central PMCID: PMC6207555.





