Osteoarthritis is characterized as a chronic condition, whereby cartilage tissue that cushions joints breaks down, causing stiffness, pain and loss of joint movement. It is a gradually occurring condition that is often perceived by patients as a nuisance and a normal symptom of aging, until the stiffness and pain become too painful to ignore. No other conditions leads to great immobility after age 65 than OA, however the joint-space narrowing may have started 20 years earlier. There is a crucial need to establish effective protocols to reduce joint damage progression at an earlier stage than when symptoms present themselves. This white paper, sponsored by Designs For Health, reviews the research on managing the metabolic processes for osteoarthritis.
White Paper Summary
Download the full text of this white paper at the end of this article.
Though the exact cause of OA is not understood, the mediators involved in functional changes and progression of the disease are understood. The pathophysiology of OA includes cartilage-degradation from enzymes, cytokines, leukotrienes (LTs) and prostaglandins (PGs). All of these mechanisms contribute to pain and inflammation in OA. This paper explains the mechanisms and the metabolic processes for osteoarthritis.
Arachidonic Pathway and NSAIDS
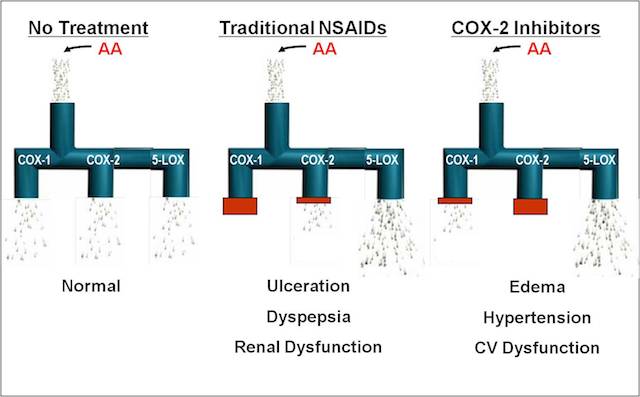
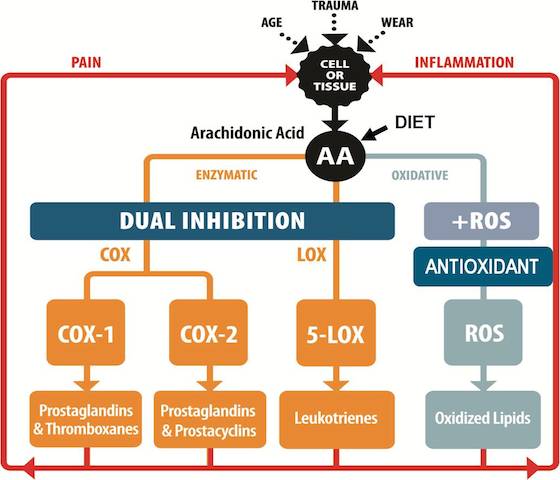
The progressive nature of OA increases production of LTs and PGs from arachidonic acid (AA), which leads to joint damage, pain and inflammation. LTs and PGs are produced by three enzymes: 5-lipoxygenase (5-LOX), cyclooxygenase COX-1 and COX-2, as part of the arachidonic acid (AA) pathway.v,vi,vii 5-LOX, along with other enzymes, converts AA to leukotrienes (LTB4, LTC4, LTD4 and LTE4) and COX-1 converts AA to thromboxanes (TXA2) and PGs (PGD2, PGE2, PGF2 and PGI2.
The AA pathway has a cascading affect. Its products and mediating enzymes are crucial to human physiology for vascular homeostasis, renal homeostasis, bone formation, and gastrointestinal protection. Yet, it can also be the cause of unwanted pain and inflammation in OA because disruptions of the AA pathway can lead to pro-inflammatory complications, particularly in the gastric system. The primary mechanism of pain relief for NSAIDs and selective COX-2 inhibitors is to disrupt the AA pathway. This may well reduce pain, but it may also lead to unwanted side effects.
Flavonoids and Inflammation
It is believed that when one increases flavonoids and omega-3 polyunsaturated acid intake, it decreases the production of inflammatory mediators and thus, the incidence and progression of OA. These observations and others substantiate the fact that dietary habits contribute to the metabolic and inflammatory etiology of OA. However, the challenge is how to balance the inhibition of COX-1, COX-2 and 5-LOX metabolic pathways. One answer lies in specific flavonoids from the botanicals, Scutellaria baicalensis and Acacia catechu. Each has been studied for their role in managing the pathways of AA metabolism.
Preclinical and clinical evidence suggests that a specialized compound of Scutellaria baicalensis and Acacia catechu, called flavocoxid, provides effective dietary management of the principal metabolic processes of OA. Flavocoxid is a medical food available by prescription for the dietary management of OA. It is a proprietary blend of two flavonoids, baicalin and catechins, derived from the botanicals Scutellaria baicalensis and Acacia catechu respectively. In a specific combination the flavonoids baicalin and catechin, extracted from Scutellaria baicalensis and Acacia catechu, inhibit phospholipase A2 (PLA2), peroxidase activity of COX-1, COX-2, and 5-LOX.
In a randomized, double-blind, active-comparator study of flavocoxid against naproxen, flavocoxid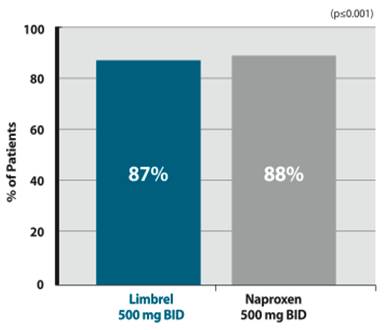
showed a favorable response. When 220 subjects with moderate to severe OA of the knee were given flavocoxid twice-daily, both groups noted a significant reduction in the signs and symptoms of OA. There were no detectable differences in efficacy between the groups. This study was significant as it offered physicians a reliable alternative to NSAIDs for OA.
DOWNLOAD THE FULL TEXT WHITE PAPER