It is commonly known that colorectal cancer risk is greater for first-degree relatives (FDR) of patients with colorectal cancer than the general population. Screening guidelines recommend a colonoscopy every 5 or 10 years beginning at the age of 40, which is dependent on whether colorectal cancer index-case is diagnosed at <60 or ≥60 y, respectively. Previous studies on whether the risk of neoplastic lesions have been inconclusive. This new study was designed to establish a better indication of risk of advanced neoplasia (three or more non-advanced adenomas, advanced adenoma, or invasive cancer) in FDR of patients with colorectal cancer compared to average-risk individuals (i.e., asymptomatic adults 50 to 69 y of age with no family history of colorectal cancer). Published May 3, 2016, PLOS medicine.

The familial stratified group was defined as follows:
- Familial-risk group was stratified as one FDR, with one family member diagnosed with colorectal cancer at ≥60 y (n = 1,884) or at <60 y (n = 831), and
- As two FDR, with two family members diagnosed with colorectal cancer at any age (n = 300).
Multiple logistic regression analysis was used for between-group comparisons after adjusting for potential confounders (age, gender, and center). Compared with the average-risk group, advanced neoplasia was significantly more prevalent:
- In individuals having two FDR with colorectal cancer (odds ratio [OR] 1.90; 95% confidence interval [CI] 1.36–2.66, p < 0.001),
- But not in those having one FDR with colorectal cancer diagnosed at ≥60 y (OR 1.03; 95% CI 0.83–1.27, p = 0.77) and <60 y (OR 1.19; 95% CI 0.90–1.58, p = 0.20).
- After the age of 50 y, men developed advanced neoplasia over two times more frequently than women and advanced neoplasia appeared at least ten y earlier.
- Fewer colonoscopies by 2-fold were required to detect one advanced neoplasia in men than in women.
According the researchers, the key findings included the following:
- The number of index-cases was 2,474 (median age 66.2 y). Of these, 1,399 (56.5%) were male and 786 (31.7%) were aged <60 y at diagnosis of colorectal cancer. Siblings with colorectal cancer predominated among individuals having two FDR affected compared to individuals having only one FDR with colorectal cancer (77.7% versus 25.5%, p < 0.001) Compared to average risk individuals, mean age of the familial-risk individuals was lower (51.8 ± 9.0 versus 59.3 ± 5.5 y, p < 0.001), as was the proportion of men (41.3% versus 47.6%, p < 0.001), as shown in Excerpt from the study.
- Men and women having two FDR with colorectal cancer showed a significantly greater risk of advanced adenomas and advanced neoplasia than those with average-risk.
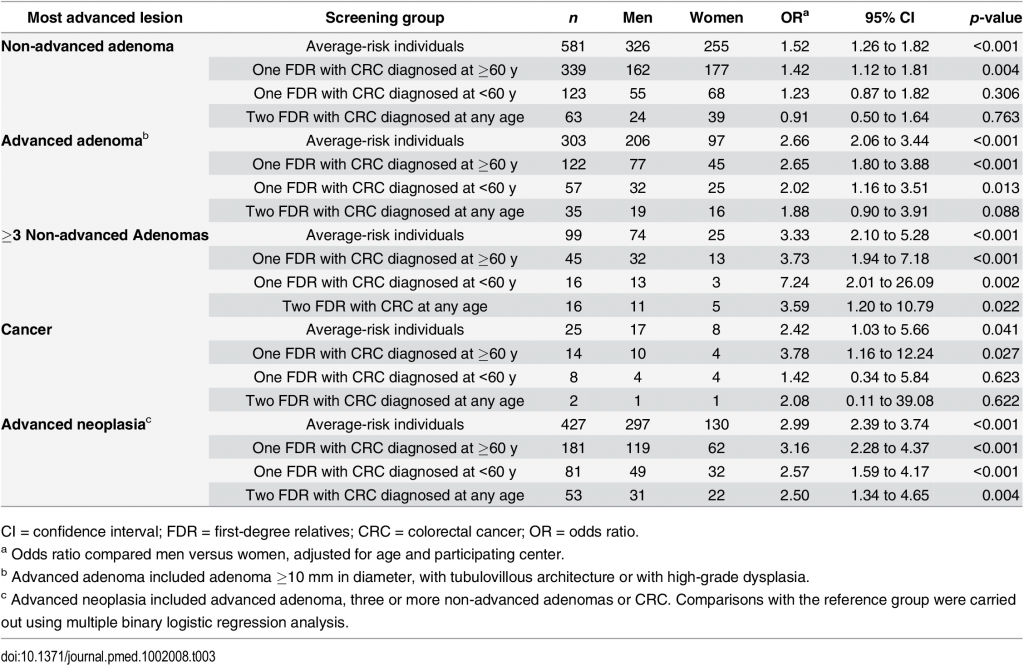
- In contrast, men and women having one FDR with colorectal cancer showed a similar risk of these lesions to average-risk individuals, regardless of index-case age at diagnosis of colorectal cancer. The risk of advanced neoplasia was almost 3-fold higher and appeared at least 10 y earlier in men than in women in both the familial- and average-risk groups. See Table 3 below.
- The number of colonoscopies needed to detect one advanced neoplasia was 2-fold higher in women than in men at all ages in both cohorts. Taken together, our results support the notion that screening colonoscopy may be delayed at least 10 y in women having one or even two FDR with colorectal cancer, as has been shown for women in the average-risk population.
CONCLUSION
“Men and women having two FDR with colorectal cancer showed a significantly greater risk of advanced adenomas and advanced neoplasia than those with average-risk. In contrast, men and women having one FDR with colorectal cancer showed a similar risk of these lesions to average-risk individuals, regardless of index-case age at diagnosis of colorectal cancer. The risk of advanced neoplasia was almost 3-fold higher and appeared at least 10 y earlier in men than in women in both the familial- and average-risk groups.”
TABLE 3