COVID-19 patients with extremely high levels of the stress hormone cortisol in their blood are more likely to deteriorate quickly and die, according to new research in Lancet.
The study, led by NIHR Research Professor Waljit Dhillo from Imperial College London and Consultant Endocrinologist at Imperial College Healthcare NHS Trust, provides the first data to show that cortisol levels are a marker of the severity of the illness. The researchers suggest they can be used to identify those patients who are more likely to need intensive care.]
The study, published in The Lancet Diabetes & Endocrinology and funded by the National Institute for Health Research (NIHR) and the Medical Research Council, involved 535 patients admitted to three London hospitals – Charing Cross, Hammersmith and St Mary’s – with suspected COVID-19 between 09 March and 22 April 2020. A COVID-19 swab test and routine blood tests – including a baseline measurement of cortisol levels – were performed within 48 hrs of admission.
As a reminder, cortisol levels when healthy and resting are 100-200 nm/L and nearly zero when we sleep.When ill patients have low levels of cortisol, it can be life threatening. Excessive levels of cortisol during illness can be equally dangerous, leading to increased risk of infection and poor outcomes.
In the new observational study of 535 patients, of whom 403 were confirmed to have COVID-19, cortisol levels in patients with COVID-19 were significantly higher than in those without:
- The levels in the COVID-19 group ranged as high as 3241 – considerably higher even than after major surgery, when levels can top 1000.
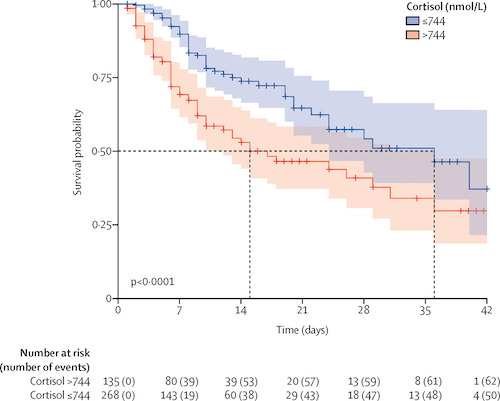
- Amongst the COVID-19 patients, those with a baseline cortisol level of 744 or less survived on average for 36 days. Patients with levels over 744 had an average survival of just 15 days.
- Over the study period, just under 27 per cent of the COVID-19 group died during the study period compared to just under 7 percent of the non-COVID-19 group.
“From an endocrinologist’s perspective, it makes sense that those COVID-19 patients who are the sickest will have higher levels of cortisol, but these levels are worryingly high,” said Professor Dhillo, Head of Division of Diabetes, Endocrinology and Metabolism at Imperial College London.
“Three months ago when we started seeing this wave of COVID-19 patients here in London hospitals, we had very little information about how to best triage people. Now, when people arrive at hospital, we potentially have another simple marker to use alongside oxygen saturation levels to help us identify which patients need to be admitted immediately, and which may not. Having an early indicator of which patients may deteriorate more quickly will help us with providing the best level of care as quickly as possible, as well as helping manage the pressure on the NHS. In addition, we can also take cortisol levels into account when we are working out how best to treat our patients.”
Conclusion/ Professor Dhillo and his team hope that their findings can now be validated in a larger scale clinical study. He writes: “Our data suggest that it is appropriate for patients with hypoadrenalism—a situation quite commonly encountered in the 3% of the population taking systemic glucocorticoid therapy5— to take or be given supplemental glucocorticoids at a high dose to prevent an acute adrenal crisis if they acquire a SARS-CoV-2 infection. Furthermore, we found that high cortisol concentrations were associated with increased mortality and a reduced median survival, probably because this is a marker of the severity of illness.6 In our cohort, cortisol seemed to be a better independent predictor than were other laboratory markers associated with COVID-19, such as CRP, D-dimer, and neutrophil to leukocyte ratio.” Read the full study for exceptions and caveats to this conclusion.
Click Here for Full Text Study





