Diabetes remission, without drugs, is possible, according to this just published Lancet study. Researchers found that nearly half of of the study subjects achieved and maintained diabetes remission at one year without anti-diabetic medications. Subjects with diabetes for as long as 6 years were able to reverse diabetes following an 8-week, low-calorie diet and intensive-weight management program.
The study has widespread public health implications for intervention therapy as a routine protocol. The key finding was that weight loss is a significant driver for reaching a non-diabetic state. After 1 year, participants had a mean weight loss of 16.9kg, and nearly half reverted to a diabetes remission without using any diabetes treatment.
Our findings suggest that even if you have had type 2 diabetes for 6 years, putting the disease into remission is feasible”, says Professor Michael Lean from the University of Glasgow who co-led the study. “In contrast to other approaches, we focus on the need for long-term maintenance of weight loss through diet and exercise and encourage flexibility to optimize individual results.”
The Diabetes Remission Clinical Trial (DiRECT), included 298 adults aged 20–65 years, who had been diagnosed with type 2 diabetes in the past 6 years from 49 primary care practices across Scotland and the Tyneside region of England between July 2014 and August 2016 (click here for a pdf of the DiRECT pre-trial protocol).
A summary of the results:
- Weight fell (98.0 ± 2.6 to 83.8 ± 2.4 kg) and remained stable over 6 months (84.7 ± 2.5 kg).
- Twelve of 30 participants achieved fasting plasma glucose <7 mmol/L after return to isocaloric diet (responders), and 13 of 30 after 6 months.
- Responders had a shorter duration of diabetes and a higher initial fasting plasma insulin level.
- HbA1c fell from 7.1 ± 0.3 to 5.8 ± 0.2% (55 ± 4 to 40 ± 2 mmol/mol) in responders (P < 0.001) and from 8.4 ± 0.3 to 8.0 ± 0.5% (68 ± 3 to 64 ± 5 mmol/mol) in nonresponders, remaining constant at 6 months (5.9 ± 0.2 and 7.8 ± 0.3% [41 ± 2 and 62 ± 3 mmol/mol], respectively).
- The responders were characterized by return of first-phase insulin response.
Rather than addressing the root cause, management guidelines for type 2 diabetes focus on reducing blood sugar levels through drug treatments. Diet and lifestyle are touched upon but diabetes remission by cutting calories is rarely discussed,” said Professor Roy Taylor from Newcastle University, UK, who co-led the study.
The study is unique in that subjects were asked to only change their diet and not 
Previous research by the same team confirmed the Twin Cycle Hypothesis—that type 2 diabetes is caused by excess fat within the liver and pancreas—and established that people with the disease can be returned to normal glucose control by consuming a very low calorie diet. However, until now, it was not known whether this type of intensive weight management was both practicable and whether it would achieve remission of type 2 diabetes in routine primary care setting.
Patient Compliance
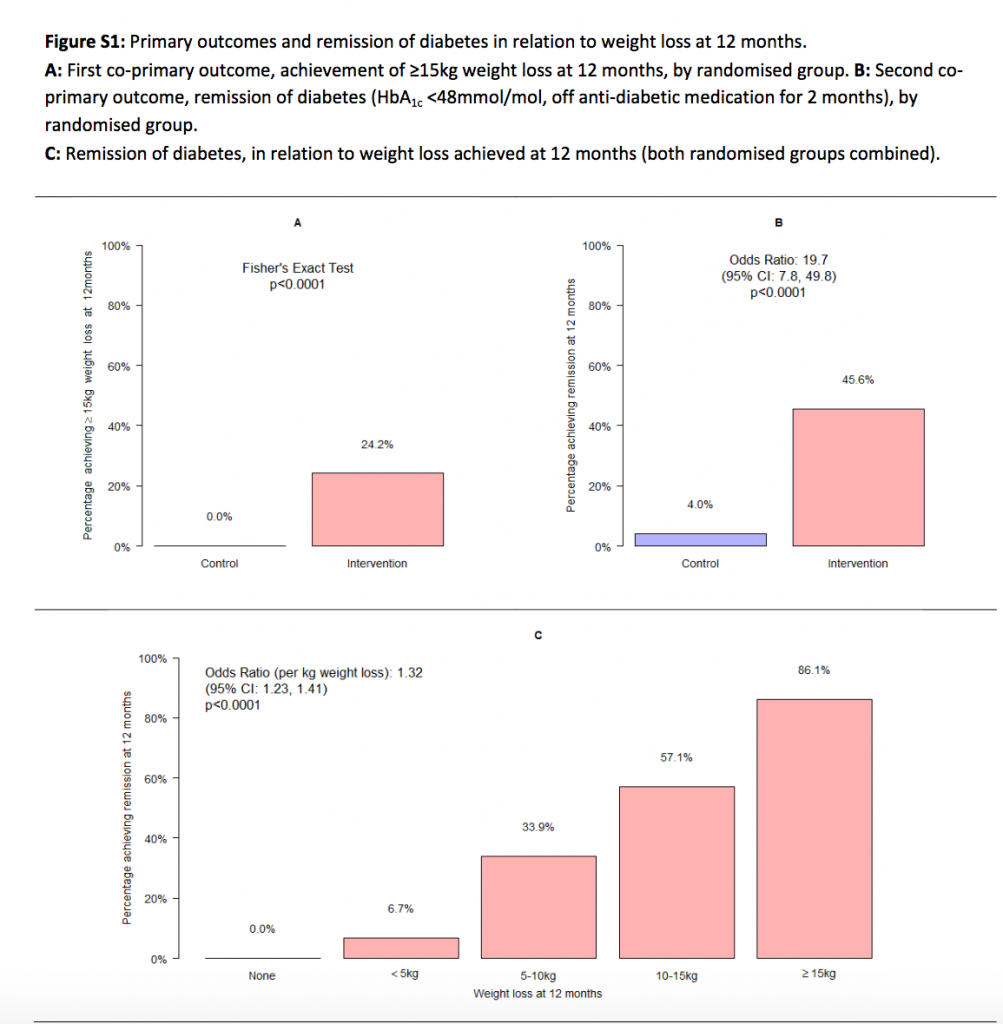
The primary outcomes were weight loss of 15 kg or more (sufficient to achieve remission of diabetes in most cases), and remission of diabetes. Remission was defined as achievement of a glycated hemoglobin A1c (HbA1c) level of less than 6.5% at 12 months, off all medications.
The weight loss program was acceptable to most participants, with a dropout rate of 21%, mainly for social reasons (e.g., bereavement, change or loss of job, moving house). 128 (86%) participants in the weight management group and 147 (99%) participants in the control group attended the 12 month assessment. For those whose measurements of weight and HbA1c level were not available it was assumed that no remission had occurred.
Lean and colleagues’ results, in addition to those from other studies of type 2 diabetes prevention and some smaller interventions in this setting, indicate that weight loss should be the primary goal in the treatment of type 2 diabetes,” wrote Professor Emeritus Matti Uusitupa from the University of Eastern Finland in a commentary. The DiRECT study indicates that the time of diabetes diagnosis is the best point to start weight reduction and lifestyle changes because motivation of a patient is usually high and can be enhanced by the professional health-care providers.”
Weight Loss
Almost a quarter (36/149) of the weight management group achieved weight loss of 15 kg or more at 12 months, compared with none in the control group. Additionally, nearly half of the weight management group (68/149) achieved diabetes remission at 1 year, compared with six (4%) in the control group.
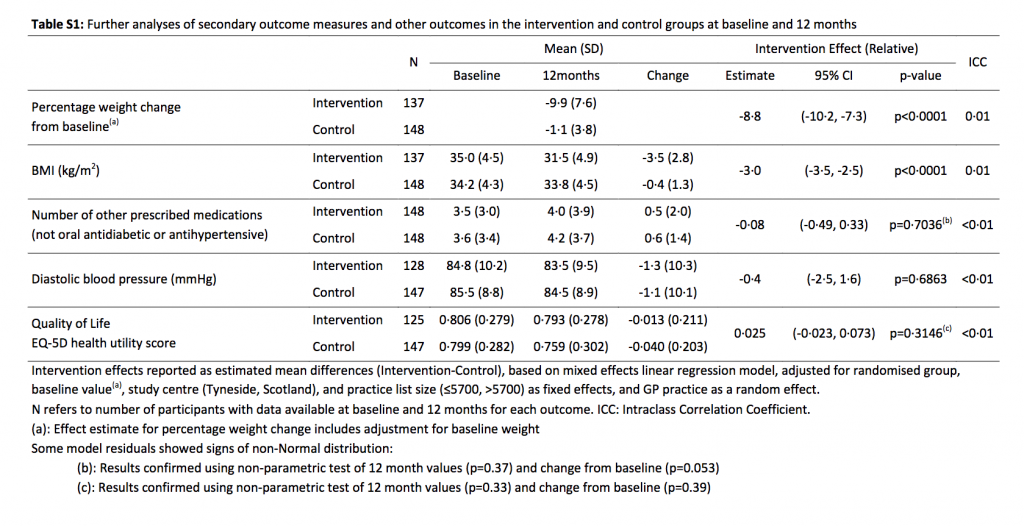
On average, participants in the weight management group shed 10kg of body weight compared to 1kg in the control group. Importantly, the results showed that remission was closely linked with the degree of weight loss and occurred in around 9 out of 10 people who lost 15 kg or more, and nearly three quarters (47/64) of those who lost 10kg or more.
The researchers also noted an improvement in average triglyceride (blood lipid) concentrations in the weight management group, and almost half remained off all anti-hypertensive drugs with no rise in blood pressure. Furthermore, the weight management group reported substantially improved quality of life at 12 months, with a slight decrease reported in the control group.
 Study Limitations
Study Limitations
Overall, one person experienced serious adverse events possibly related to the treatment (biliary colic and abdominal pain) but continued in the study. Some participants experienced constipation, headache, and dizziness.
The authors note that the vast majority of participants were white and British, meaning that the findings may not apply to other ethnic and racial groups such as south Asians, who tend to develop diabetes with less weight gain.
Conclusion
“Our findings suggest that the very large weight losses targeted by bariatric surgery are not essential to reverse the underlying processes which cause type 2 diabetes. The weight loss goals provided by this programme are achievable for many people. The big challenge is long-term avoidance of weight re-gain. Follow-up of DiRECT will continue for 4 years and reveal whether weight loss and remission is achievable in the long-term,” said Professor Taylor.
For More on the DiRECT Study, published in Lancet, Click Here.