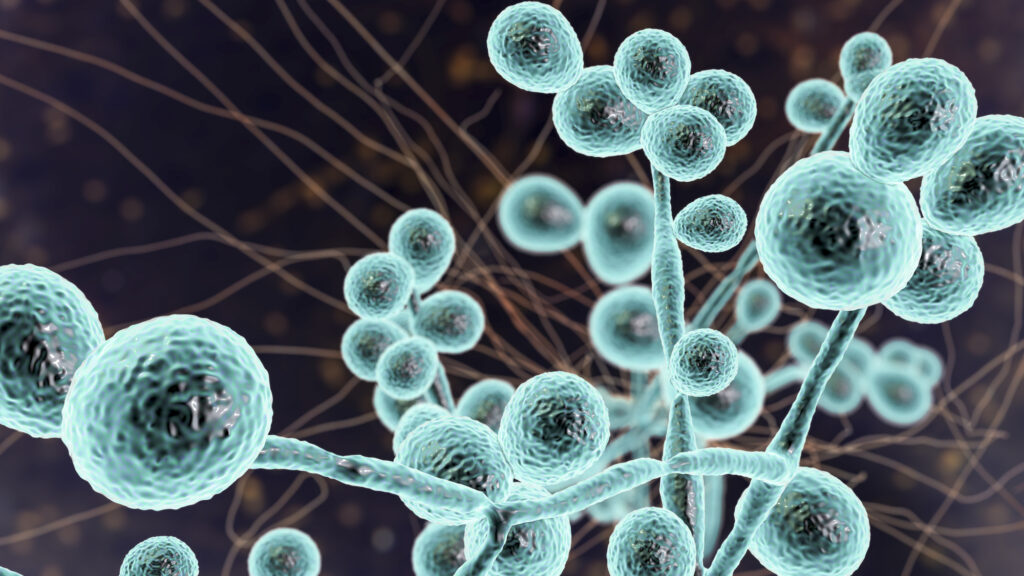
Candida is a yeast often found on the skin and in the digestive tract of healthy people. Some species, such as Candida albicans, occasionally grow out of control and cause mild infections. In more serious cases, however, Candida can invade deep into the body and cause infections in the bloodstream or organs such as the kidney, heart, or brain. Immunocompromised people, including many hospital patients, are most at risk for invasive Candida infections, which are rapidly evolving drug resistance.
In 2009, a new Candida species, C. auris, emerged in a hospital patient in Japan. Since then, C. auris has caused outbreaks in more than a dozen countries around the world with more than 3,000 clinical cases reported in the United States alone. To make matters worse, C. auris is often multidrug-resistant and has a high mortality rate—estimates range from 30% to 60%—leading the Centers for Disease Control and Prevention (CDC) to label it a serious global health threat.
To combat this emerging threat, scientists are exploring a number of different possibilities. “Drug-resistant fungal infections are a growing healthcare problem but there are few new antifungals in the drug-development pipeline,” says Cassandra Quave, PhD, assistant professor at the Emory University School of Medicine and senior author of a new study identifying one such antifungal. “Our findings open a new potential approach to deal with these infections, including those caused by deadly Candida auris.” Quave and her team published their results in the journal ACS Infectious Diseases.
The Study
Previously, Quave found that the berries of the Brazilian peppertree, a plant used by traditional healers to treat skin infections, contain a flavone-rich compound that disarms drug-resistant staph bacteria. From there, Quave isolated a compound in the plant’s leaves known as PGG, which showed antibacterial, anticancer, and antiviral activities. With those results in hand, Quave decided to test whether PGG would also show antifungal activity against Candida.
Laboratory-dish experiments demonstrated that PGG did, indeed, show antifungal activity. In fact, it blocked about 90% of the growth in 12 strains from four species of Candida: C. albicans, multidrug-resistant C. auris, and two other multidrug-resistant non-albicans Candida species.
PGG works, Quave’s team discovered, by depriving Candida of iron. “Each PGG molecule can bind up to five iron molecules,” says Lewis Marquez, a graduate student at Emory and another of the study’s authors. “When we added more iron to a dish, beyond the sequestering capacity of the PGG molecules, the fungi once again grew normally.”
Because it starves Candida rather than attacking it, the researchers say that PGG won’t promote the development of further drug resistance like existing antifungals do. Laboratory-dish experiments also showed minimal toxicity of PGG to human cells.
Conclusions
Previous animal studies on PGG have found that the molecule is metabolized quickly and removed from the body, so the team first intends to explore its potential efficacy as a topical treatment. “If a Candida infection breaks out on the skin of a patient where a catheter or other medical instrument is implanted, a topical antifungal might prevent the infection from spreading and entering into the body,” Marquez says. With that in mind, the researchers plan to test PGG on fungal skin infections in mice.
Meanwhile, Quave and Marquez have applied for a provisional patent for the use of PGG for the mitigation of fungal infections. “These are still early days in the research, but another idea that we’re interested in pursuing is the potential use of PGG as a broad-spectrum antimicrobial,” Quave says. “Many infections from acute injuries, such as battlefield wounds, tend to be polymicrobial, so PGG could perhaps make a useful topical treatment in these cases.”