“We’re Last! Again!” was the headline on NBC News regarding the most recent Commonwealth Fund Report on the state of industrialized countries’ healthcare systems. Once again, the US was deemed the most expensive and the least effective, least equitable and had the poorest outcomes among its economic counterparts. Critics argued the study is biased toward socialized medicine and does not take into account the technological advances and patient satisfaction and outcomes.
On the plus side, the US scored well in preventive care efforts, under the category of “effective care.” And, certain states scored well —Minnesota, Massachusetts, New Hampshire, Vermont, and Hawaii—lead the nation across most dimensions of care.
The study, report Mirror, Mirror on the Wall: How the Performance of the U.S. Health Care System Compares Internationally, 2014 Update, which was done prior to the Affordable Health Care Act, showed Americans spend more in medical care ($8,508 per person) than the other 10 countries. And despite the higher spend, it’s less efficient and worse yet, Americans lives are shorter in comparison.
Summary of the findings:
Healthy lives: The U.S. does poorly, ranking last on infant mortality and on deaths that were potentially preventable with timely access to effective health care and second-to-last on healthy life expectancy at age 60.
Health care quality: The U.S ranks in the middle. On two of four measures of quality—effective care and patient-centered care—the U.S. ranks near the top (3rd and 4th of 11 countries, respectively), but it does not perform as well providing safe or coordinated care.
Efficiency: The U.S ranks last, due to low marks on the time and dollars spent dealing with insurance administration, lack of communication among health care providers, and duplicative medical testing. Forty percent of U.S. adults who had visited an emergency room reported they could have been treated by a regular doctor, had one been available. This is more than double the rate of patients in the U.K. (16%).
Equity: The U.S. ranks last. About four of 10 (39%) adults with below-average incomes in the U.S. reported a medical problem but did not visit a doctor in the past year because of costs, compared with less than one of 10 in the U.K., Sweden, Canada, and Norway. There were also large discrepancies between the length of time U.S. adults waited for specialist, emergency, and after-hours care compared with higher-income adults.
The study authors say the United States’ ranking was pulled down substantially because of deficiencies in access to primary care and inequities and inefficiencies in our health care system. Since the report data was collected prior to the Affordable Care Act, the data may improve in the future, the study authors noted. “Now that millions more Americans have good coverage, we have to invest in our health care delivery system to be sure all patients—and especially those with the greatest need and whose care is the most costly—can get the high-quality, well-coordinated health care they need,” said Commonwealth Fund President David Blumenthal, M.D. “Those kinds of improvements will go a long way toward improving peoples’ health while making efficient use of our precious health care dollars.”
Overall, when compared to other countries, people in the U.S. had the most difficulty affording health care. The report ranked the U.S. last on every measure of cost-related access. More than one-third (37%) of U.S. adults reported forgoing a recommended test, treatment, or follow-up care because of cost.
In response to the report Philip Klein of the Washington Examiner says the study is “rigged to produce a result that favors socialized health care systems. The study determines that the U.S. system is worse because it lacks universal health insurance coverage and the report emphasizes ‘equity’ as one of the key factors in evaluating a health care system.”
Klein argues this is an “ideological decision,” and goes on to say the study does not take into account medical innovation, patient satisfaction or cancer outcomes. Klein also says the report fails to address patient satisfaction and even patient neglect, which have been reported in the news the UK.
The report called out individual states with the best and poorest performance. The top quartile states included Colorado, South Dakota, Minnesota, Iowa, Wisconsin, Vermont, New Jersey, Maine, Massachusetts, New Hampshire, Connecticut, Rhode Island, Delaware and Hawaii. At the end of this article, download summaries of each state’s rankings.
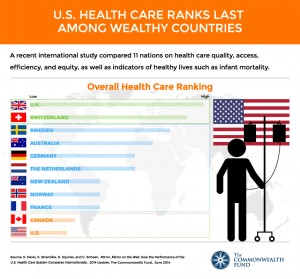
The full rankings are as follows:
1. United Kingdom
2. Switzerland
3. Sweden
4. Australia
5. Germany & Netherlands (tied)
7. New Zealand & Norway (tied)
9. France
10. Canada
11. United States
DOWNLOAD STATE HEALTHCARE PROFILES