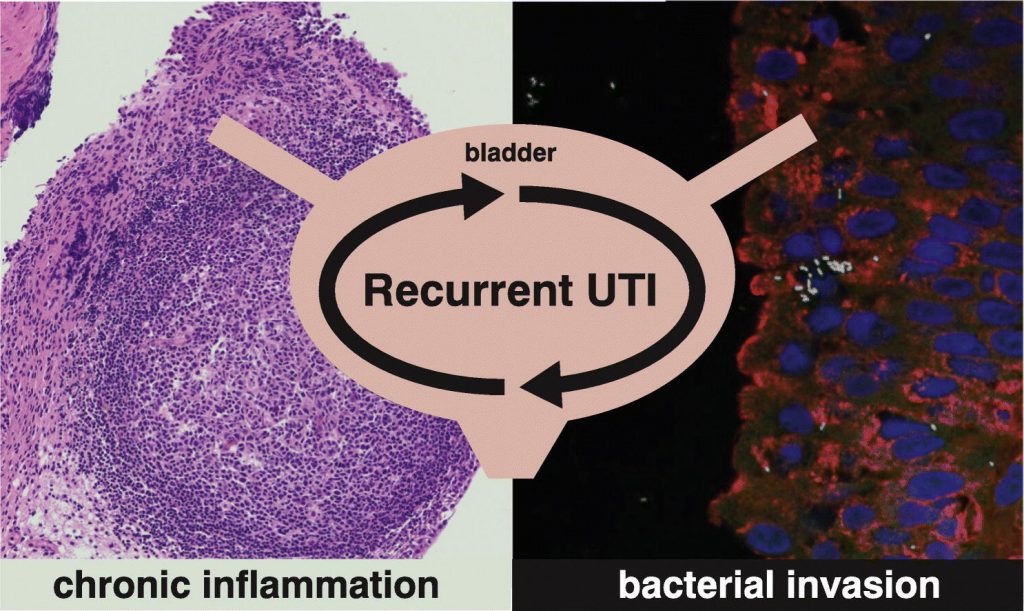
A new finding shows that several species of bacteria reside in bladder tissue of postmenopausal women who experience recurrent urinary tract infections (RUTIs). The results represent the first systematic analysis of biopsies from patients in this population. A new finding by researchers at The University of Texas at Dallas and UT Southwestern Medical Center shows that several species of bacteria reside in bladder tissue of postmenopausal women who experience RUTIs.
The results, published online April 17 in the Journal of Molecular Biology, provide a better understanding of the interaction between bacteria and host tissue, which might lead to more effective treatment strategies.
The majority of UTIs are caused by the bacterium Escherichia coli, which normally lives in human intestines but sometimes gets into the urinary tract, where it is not welcome. The infections, which predominantly occur in women, typically can be treated effectively with antibiotics. But for some postmenopausal women, UTIs recur so frequently that they become a chronic condition, requiring daily doses of increasingly powerful antibiotics as the infection-causing bacteria gradually become resistant to each new drug.
“For older women, these infections can go on for tens of years,” said Dr. Nicole De Nisco, assistant professor of biological sciences at UT Dallas and lead author of the study. “Eventually, a patient’s last resort might be removing the bladder.”
Most of the epidemiological research on UTIs has been done with women in their 20s and 30s, a much earlier age range than the typical onset of menopause. To investigate the pathogenic mechanisms and immune responses related to recurring UTIs, De Nisco and her colleagues analyzed urine and biopsies from 14 postmenopausal women who had undergone cystoscopy with fulguration of trigonitis, a procedure aimed at treating antibiotic-resistant UTIs by removing inflamed bladder tissue.
“One of the reasons urinary tract infections have been overlooked is because they affect women, an understudied group in general when it comes to disease, and older women in particular, who are even more understudied,” De Nisco said.
ABSTRACT/ Because treatment of RUTI by long-term antibiotic therapy is often ineffective or poorly tolerated in elderly women, new therapies must be developed. The molecular basis of RUTI, especially in postmenopausal women, has remained unclear because modeling RUTI in mice is difficult, and human data are limited. Invasion of the urothelium and induction of host inflammation are hypothesized to be key mechanisms by which bacterial pathogens cause RUTI.
To further our understanding of RUTI in humans, we performed a systematic analysis of 
Histopathological scoring revealed significant edema and alterations of urothelial architecture in RUTI patient biopsies. Lymphocytes, including plasma B-cells, were detected within the mesenchyme, urothelium, and follicular aggregates in the majority of patients, indicating that the local adaptive immune response is active during human RUTI. These data provide conclusive evidence that bacteria invade the human urothelium and suggest that diverse bacterial species and the adaptive immune response play important roles in RUTI in humans.
They found that in addition to the expected E. coli, bacteria in urine samples included Klebsiella pneumoniae and Enterococcus faecalis, while species in biopsied tissue included E. coli, Staphylococcus hominis and Bacillus firmus.
“Our findings confirm that bacteria do form communities within the bladder wall of RUTI patients, which was not previously known,” De Nisco said. “This research is a critical step toward better understanding the mechanisms of recurring urinary tract infection and inflammation in postmenopausal women.”