As poor nutritional status affects more and more children, researchers are beginning to see dramatic health ramifications. For instance, in this study at Boston Medical Center, published in the journal Hypertension, researchers looked at persistent low vitamin D in newborns to early childhood to see how it might be associated with higher risk of elevated blood pressure from ages 3 to 18.
The study followed 775 children of low income families from birth to age 18. Cord blood was drawn at birth to analyze the levels of vitamin D in newborns.
Optimum levels of vitamin D in pregnancy and early life remains a controversial matter. However, in this study less than 11ng/ml was defined as low at birth and less than 25ng/ml was defined as low in early childhood.

“Our findings raise the possibility that screening and treatment of vitamin D deficiency with supplementation during pregnancy and early childhood might be an effective approach to reduce high blood pressure later in life.” ~ Guoying Wang, M.D, Ph.D, lead author.
The results revealed ramifications of low vitamin D at birth throughout the life of the child.
- Low levels of vitamin D at birth correlated with a 60% chance of high systolic blood pressure between ages 6 and 18.
- Overall, 44.3% and 23.0% children had low 25(OH)D concentrations at birth and during early childhood, respectively,
- Also, 11.4% children had persistent low vitamin D status from birth to early childhood.
- Maternal hypertension disorder and childhood OWO were more common in the elevated SBP group. Children with elevated SBP had lower birthweight, gestational age, and low 25(OH)D concentrations.
- Of the mothers with child who had SBP <75 percentiles or SBP ≥75 percentiles, 48.6% and 46.4% had taken prenatal vitamins (containing 400 IU vitamin D) almost daily in the third trimester, respectively.
- It is important to note that 68% of the children in the study were African American, which supports previous research that people with darker skin may require more vitamin D due to the additional melanin in the skin, which reduces the ability to absorb vitamin D from the sun.
- The new study parallels previous findings where over 90% of premature babies were found to have low vitamin D levels suggesting low vitamin D during pregnancy and early life is detrimental to healthy development.
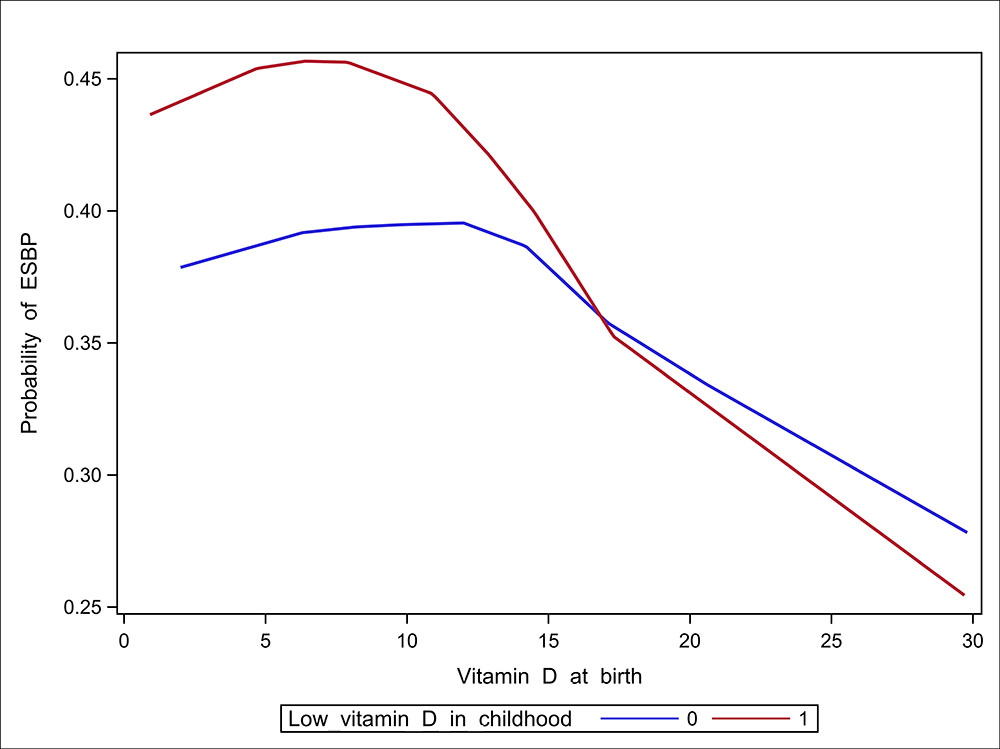
The researchers note that persistently low vitamin D was associated with elevated SBP above and beyond established hypertension risk factors. These associations were particularly stronger among schoolchildren and adolescents. Low vitamin D status at birth or in early childhood was also independently associated with elevated SBP, and the higher risk was particularly evident among children whose mothers had cardiometabolic conditions. See FIGURE 1.
FIGURE 1
Clinical Ramifications
These findings highlight that both prenatal and early childhood vitamin D levels appear to play a substantial role in the development of elevated SBP, especially among those born to mothers with obesity, diabetes mellitus, or hypertensive disorders.
This study is evidence that there is a need for a preventive role of optimal prenatal and postnatal vitamin D levels on SBP in childhood and adolescence. “Optimal vitamin D levels could be essential as early as in utero for the risk reduction of elevated SBP. Screening for vitamin D levels during pregnancy or the first years of life should be recommended for pregnant women and their babies who are at a high risk, such as those with cardiometabolic risk conditions, so that they receive appropriate treatment and monitoring,” the researchers note.
Conclusion/ “This work underscores that the perinatal and early childhood periods are critical windows for nutritional interventions aimed at preventing the development of hypertension in late life,” the researchers write.
“Further clinical and experimental studies may be warranted to validate our findings. If our findings are confirmed, prenatal and early childhood screening and optimal vitamin D supplementation may form a cost-effective approach to reduce the risk of hypertension and CVD later in life, given the safe and low cost of treating vitamin D deficiency, especially in black or obese populations.”